Diabetes mellitus is a chronic condition that affects millions of people worldwide, characterized by the body’s inability to regulate blood sugar (glucose) levels properly.
There are two primary types of diabetes: Type 1 vs. Type 2 diabetes. Although both types lead to high blood sugar levels and share some common symptoms, their underlying causes, development, and specific symptoms differ significantly.
At Catholicfating, understanding these differences is crucial for effective diagnosis, treatment, and management.
What is Type 1 diabetes?
Type 1 diabetes, previously called juvenile-onset or insulin-dependent diabetes, is an autoimmune disease that can occur in children and adults at any age.
For reasons that are not yet entirely understood, the immune system, the body’s defense against infection, mistakenly attacks and destroys the insulin-producing beta cells in the pancreas. Scientists believe that genetics and environmental factors, such as a virus, trigger the disease. Its onset, which can be sudden, is not related to diet or lifestyle.

As a result, the body produces little to no insulin to regulate blood sugar and get energy from food. Glucose is locked out of the cells, leading to high levels in the bloodstream.
If you have type 1 diabetes, you will need to take daily insulin shots or wear an insulin pump to manage your glucose levels and ensure your body gets the energy it needs. You can’t take insulin as a pill because the acid in the stomach would destroy it.
You must check your blood sugar often, even overnight, and closely watch what you eat to avoid potentially dangerous spikes and lows.
Symptoms of Type 1 Diabetes
Type 1 diabetes symptoms can appear suddenly and may include:
- Feeling thirstier than usual
- Urinating a lot
- Bed-wetting in children who have never wet the bed during the night
- Feeling very hungry
- Losing weight without trying
- Feeling irritable or having other mood changes
- Feeling tired and weak
- Having blurry vision
Causes of type 1 diabetes
- The body’s immune system is responsible for fighting off foreign invaders, such as harmful viruses and bacteria.
- Type 1 diabetes is believed to be caused by an autoimmune reaction. In people with type 1 diabetes, the immune system mistakes the body’s healthy cells for foreign invaders.
- The immune system attacks and destroys the insulin-producing beta cells in the pancreas. After these beta cells are destroyed, the body is unable to produce insulin.
- Researchers don’t know why the immune system sometimes attacks the body’s cells. It may have something to do with genetic and environmental factors, such as exposure to viruses.
- Research into autoimmune diseases is ongoing. Diet and lifestyle habits do not cause type 1 diabetes.
What is Type 2 diabetes?
Type 2 is the most common form of diabetes, accounting for 90 to 95% of people diagnosed.
Type 2 diabetes can result when the pancreas is producing insulin, but the cells are not responding to it the way they should. As opposed to type 1 diabetes, where there’s no insulin key to open the cells, with type 2 diabetes, the locks on the cells are damaged.
Less glucose can enter the cells, leading to high levels in the bloodstream. This is called insulin resistance. In response, the pancreas works harder to make more insulin to force the cells open. Over time, this can damage the pancreas, and it may not be able to produce any insulin.

As the disease progresses and the beta cells in your pancreas cease insulin production, you will need to begin insulin injections. (This does not mean you now have type 1 diabetes, as the two conditions have different causes.)
Because your body is not getting the energy it needs, constant hunger and excessive thirst are often among the first symptoms of type 1 and type 2 diabetes. Other early signs include:
- Lack of energy and fatigue
- Frequent urination
- Blurry vision
- Unintended weight loss
- Cuts and bruises that are slow to heal
- Tingling, pain, or numbness in the hands and feet (type 2)
While the onset of type 1 diabetes can be sudden, with type 2, the symptoms can come on gradually and may be easy to dismiss. Over time, however, symptoms become more severe and lead to complications like loss of feeling in your extremities (neuropathy), kidney disease, vision loss, heart attack, and stroke.
Type 2 diabetes may run in families, but you are more likely to develop it if you are obese or overweight, lead a sedentary lifestyle, eat high-fat, high-sugar foods, have high blood pressure, and have low HDL cholesterol and/or high triglycerides. In women, diabetes during pregnancy and polycystic ovary syndrome are also risk factors.
Type 2 diabetes is more likely to occur in people over 40. However, with increased rates of obesity, younger people are developing it as well.
Unlike type 1 diabetes, you can control and even prevent type 2 diabetes with diet and exercise. Losing 7 to 10% of your body weight can help your body use insulin more efficiently. Several medications are also available to help manage type 2 diabetes. Bariatric weight-loss surgery has also been shown to eliminate type 2 diabetes in some people.
With the right tools and support, you can manage your condition and live your life to the fullest.
Symptoms of type 2 diabetes:
A lot of people don’t get any signs or symptoms of type 2 diabetes, or don’t notice them. Symptoms can include:
- Weeping a lot, especially at night
- Being thirsty.Feeling more tired than usual. Losing weight without trying to—and getting thinner.Genital itching or thrush.
- Cuts and wounds take longer to heal.
Causes of type 2 diabetes
People with type 2 diabetes have insulin resistance. The body still produces insulin, but it’s unable to use it effectively.
Researchers aren’t sure why some people become insulin resistant and others don’t, but several lifestyle factors may contribute, including being inactive and carrying excess weight.
Other genetic and environmental factors may also play a role. When you develop type 2 diabetes, your pancreas will try to compensate by producing more insulin. Because your body is unable to effectively use insulin, glucose accumulates in your bloodstream.
Can type 2 diabetes be cured?
There isn’t a cure for type 2 diabetes or any other type of diabetes. By losing weight, some people can reverse their type 2 diabetes, known as remission.

This means their blood sugar levels are back at ‘normal’ levels rather than within the range for diabetes or prediabetes, and they don’t need to take diabetes medication to manage their blood sugar levels. But type 2 diabetes can come back if people put weight back on.
What causes diabetes?
Type 1 and type 2 diabetes may have similar names, but they’re different diseases with unique causes.
The key difference between type 1 and type 2 diabetes is that type 1 is believed to be caused by an autoimmune reaction and develops early in life. Type 2 diabetes develops over many years and is related to lifestyle factors such as being inactive and carrying excess weight. It’s usually diagnosed in adults.
Risk factors for type 1 diabetes are not as clear, but family history may play a role.
How does diabetes affect the body?
There are two main types of diabetes: type 1 and type 2.
Both types of diabetes are chronic diseases that affect the way your body regulates blood sugar or glucose. Glucose is the fuel that feeds your body’s cells, but to enter your cells, it needs a key. Insulin is the key.
People with type 1 diabetes don’t produce insulin. You can think of it as not having a key.
People with type 2 diabetes don’t respond to insulin as well as they should, and later in the disease,e often don’t make enough insulin. You can think of it as having a broken key.
Both types of diabetes can lead to chronically high blood sugar levels. That increases the risk of diabetes complications.
Risk Factors of Type 1 vs. Type 2 Diabetes
Diabetes mellitus, commonly referred to simply as diabetes, is a chronic condition characterized by elevated blood sugar levels. There are two primary types of diabetes: Type 1 vs. Type 2.
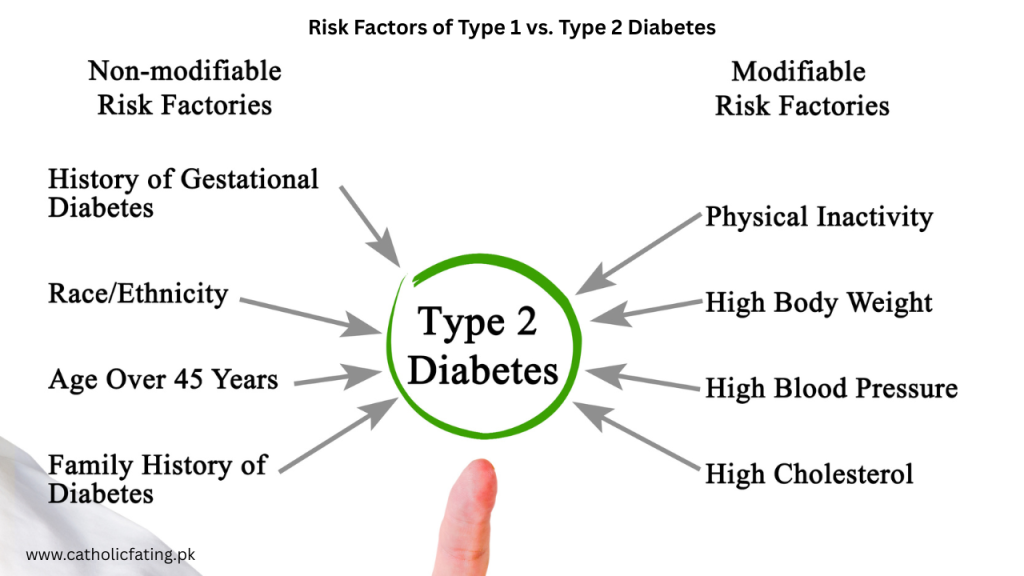
While both types involve issues with insulin, the hormone that regulates blood sugar, their causes and risk factors differ significantly.
Risk Factors of Type 1 Diabetes
Type 1 diabetes, often diagnosed in childhood or adolescence, but can occur at any age, is an autoimmune disease. This means the body’s immune system mistakenly attacks and destroys insulin-producing cells in the pancreas.
The exact cause of this autoimmune response is not fully understood, but several risk factors contribute to its development:
- Genetics: Individuals with a family history of Type 1 diabetes have a higher risk of developing the condition.
- Autoimmune Factors: Certain infections or environmental factors may trigger the autoimmune response that leads to Type 1 diabetes in genetically susceptible individuals.
- Age: Although Type 1 diabetes can occur at any age, it is most commonly diagnosed in children, adolescents, and young adults.
- Exposure to Viruses: Some viruses, such as enteroviruses and coxsackievirus, have been linked to an increased risk of Type 1 diabetes.
Risk Factors of Type 2 Diabetes
Type 2 diabetes is the most common form of diabetes, accounting for the vast majority of cases worldwide. It develops when the body becomes resistant to insulin or when the pancreas fails to produce enough insulin. Several risk factors contribute to the development of Type 2 diabetes:
- Obesity: Excess body weight, particularly abdominal obesity, significantly increases the risk of Type 2 diabetes.
- Physical Inactivity: Lack of regular physical activity is strongly associated with an increased risk of Type 2 diabetes.
- Poor Diet: Diets high in processed foods, sugar, and unhealthy fats contribute to the development of insulin resistance and Type 2 diabetes.
- Family History and Genetics: Having a family member with Type 2 diabetes increases the risk of developing the condition.
- Age: The risk of Type 2 diabetes increases with age, especially after the age of 45.
- Ethnicity: Certain ethnic groups, including African Americans, Hispanic/Latino Americans, Native Americans, and Asian Americans, have a higher risk of developing Type 2 diabetes.
- Gestational Diabetes: Women who have had gestational diabetes (diabetes during pregnancy) are at higher risk of developing Type 2 diabetes later in life.
Common Risk Factors for Both Types
While Type 1 and Type 2 diabetes have distinct causes, some risk factors are common to both types:
- Obesity: While more strongly associated with Type 2 diabetes, obesity can also increase the risk of Type 1 diabetes.
- Family History: A family history of diabetes in general, regardless of type, increases the risk of developing either Type 1 or Type 2 diabetes.
- Age: Both types of diabetes can develop at any age, but age is a general risk factor due to the cumulative effects of other risk factors over time.
- Inactivity: Lack of physical activity is detrimental to insulin sensitivity, which impacts both types of diabetes.
- Poor Diet: Diets high in sugars, fats, and processed foods contribute to insulin resistance and increase the risk of diabetes, regardless of type.
Understanding these risk factors is crucial for prevention, early detection, and management of diabetes.
Lifestyle modifications, such as maintaining a healthy weight, staying physically active, and eating a balanced diet, play a significant role in reducing the risk of developing both Type 1 and Type 2 diabetes.
Regular medical check-ups and screenings are essential, especially for individuals with a family history or other predisposing factors.
Complications of Type 1 vs. Type 2 Diabetes
Diabetes, whether Type 1 or Type 2, can lead to various complications that significantly impact health and quality of life. While both types of diabetes involve problems with insulin, they differ in their causes and onset.
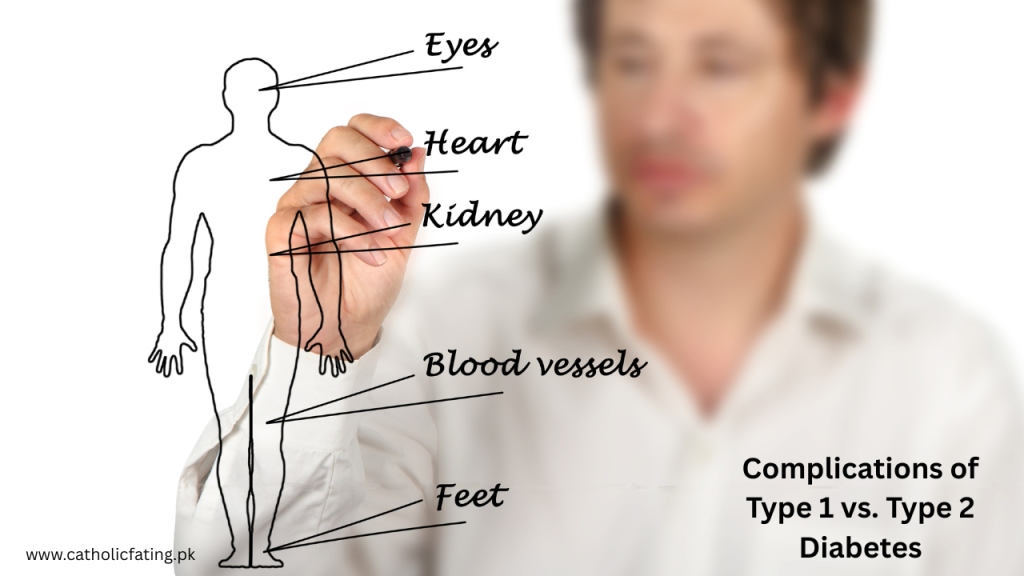
Here’s a detailed look at the complications associated with each type:
Type 1 Diabetes Complications:
Type 1 diabetes, often diagnosed in childhood or early adulthood, is characterized by the immune system attacking insulin-producing cells in the pancreas. This results in little to no insulin production.
Complications can include:
- Hypoglycemia (Low Blood Sugar): Insulin therapy can sometimes lead to blood sugar dropping too low, causing dizziness, confusion, and, in severe cases, unconsciousness.
- Diabetic ketoacidosis (DKA): Without enough insulin, the body breaks down fat for energy, leading to a buildup of acidic ketones in the blood. DKA is a medical emergency that requires immediate treatment.
- Cardiovascular Disease: People with Type 1 diabetes are at increased risk of heart disease, including heart attacks, strokes, and high blood pressure.
- Kidney Disease (Nephropathy): High blood sugar levels over time can damage the kidneys, leading to kidney failure and the need for dialysis or kidney transplantation.
- Eye Damage (Retinopathy): Diabetes can damage the blood vessels in the retina, leading to vision problems and even blindness if untreated.
- Neuropathy: Nerve damage due to diabetes can cause tingling, numbness, or pain in the hands and feet, and eventually affect digestion, sexual function, and other body systems.
Type 2 diabetes complications:
Type 2 diabetes is often linked to lifestyle factors such as obesity and lack of physical activity. It involves insulin resistance, where the body’s cells do not respond effectively to insulin.
Complications include:
- Heart Disease and Stroke: Type 2 diabetes increases the risk of cardiovascular problems, including heart attacks and strokes, due to elevated blood glucose levels damaging blood vessels over time.
- Similar to Type 1 diabetes, nerve damage can occur, particularly in the feet and legs, leading to pain, numbness, or a loss of sensation.
- Kidney Disease (Nephropathy): Diabetes is a leading cause of kidney failure. High blood sugar levels can damage the kidneys’ filtering system, leading to protein in the urine, swelling, and eventually kidney failure.
- Eye Damage (Retinopathy): Type 2 diabetes can cause damage to the blood vessels in the retina, leading to diabetic retinopathy, which can cause vision loss if left untreated.
- Foot Complications: Nerve damage and poor blood flow to the feet can lead to infections, ulcers, and, in severe cases, amputation.
- Skin Conditions: People with diabetes are more prone to skin infections and conditions, like bacterial and fungal infections.
Managing Diabetes and Reducing Complications
Managing both Type 1 and Type 2 diabetes involves maintaining blood glucose levels within a target range through a combination of insulin (for Type 1) or medication, diet, and exercise (for Type 2).
Regular monitoring of blood sugar levels, following a healthy diet, staying physically active, and taking medications as prescribed are crucial steps in reducing the risk of complications.

Moreover, routine medical check-ups, eye exams, kidney function tests, and foot examinations can help detect complications early when treatment is most effective. Lifestyle changes such as quitting smoking, managing stress, and maintaining a healthy weight also play significant roles in preventing and managing diabetes-related complications.
While diabetes can lead to serious complications affecting various organs and systems in the body, proactive management and lifestyle changes can significantly reduce the risk and severity of these complications, improving overall health and well-being for individuals living with diabetes.
What is the difference between type 1 and type 2 diabetes?
- Type 1 diabetes, once known as juvenile diabetes, is defined as the autoimmune or idiopathic destruction of β cells that causes severe insulin deficiency, in contrast to type 2 diabetes, which is characterized by insulin resistance.
- Historically, type 1 diabetes has been considered a disease that primarily affects children and adolescents (aged 10–19 years), and consequently, diagnosis, clinical care, and advocacy have largely been focused on younger populations. However, findings from recent epidemiological studies and the development of the type 1 diabetes index—a data simulation tool that estimates the number of type 1 diabetes cases for all ages across countries—have shown that the majority of incidence and prevalent cases of type 1 diabetes are in adults.
- It is estimated that up to 40% of adults older than 30 with type 1 diabetes might have been misdiagnosed with type 2 diabetes. Considering that the life expectancy of people with type 1 diabetes is reduced by up to 8 years when compared with the general population, in contrast to 3 years for people with type 2 diabetes, a paradigm shift towards a greater awareness of type 1 diabetes in adults in the clinical and research fields is needed.
The global agenda, which is overwhelmingly focused on the prevention and treatment of type 2 diabetes in adults, must be expanded to include type 1 diabetes, which has its challenges, mainly its diagnosis and subsequent appropriate treatment.
- One of the fundamental challenges with the misdiagnosis of type 1 diabetes in adults is the assumption that an adult with diabetes would have type 2 diabetes by default. Another important factor contributing to misdiagnosis is that some adults with type 1 diabetes might not need insulin at the time of diagnosis (eg, patients with latent autoimmune diabetes of adults), so their clinical disease might be masked as type 2 diabetes.
Additionally, some risk factors for type 2 diabetes, such as obesity and metabolic syndrome, are now much more common in the general population and cannot be used to rule out a diagnosis of type 1 diabetes.
Furthermore, quite often there is poor accessibility to perform diagnostic tests, such as islet autoantibodies and C-peptide measurement, that can distinguish type 1 vs. type 2 diabetes. However, it is also important to acknowledge that the diagnostic algorithm for type 1 diabetes is not as straightforward as for type 2 diabetes, which makes classification even more difficult.
- The adverse consequence of type 1 diabetes misdiagnosis is that it affects the management of the disease, which is different from type 2 diabetes, and the mismanagement negatively affects the quality of life and survival of patients. The cornerstone treatment of type 1 diabetes is intensive insulin therapy to prevent long-term complications, but treatment strategies should also aim to minimize the psychosocial burden of the disease.
Fortunately, the development of new technologies promises to achieve this. Continuous glucose monitoring (CGM), consisting of a subcutaneous sensor that continuously measures glucose levels in interstitial fluid, reduces the number of finger pricks needed and avoids fluctuations in blood glucose levels, thus providing more personalized care.
Regarding insulin delivery, different insulin pumps and hybrid closed-loop systems (also called artificial pancreas or automated insulin delivery) are safe and improve glycaemic control in youths and adults with type 1 diabetes, but require continuous user input.
Additional sophisticated technologies are currently being evaluated, such as the bionic pancreas, a fully automated closed-loop system, which is initialized only based on body weight without requiring continuous input from the user.
Although these advanced technologies are encouraging, their high cost makes them unaffordable for the majority of people with type 1 diabetes.
Conclusion
Understanding the differences in symptoms between Type 1 and Type 2 diabetes is crucial for accurate diagnosis and effective management. While both types share common symptoms, their distinct causes and specific symptoms necessitate different approaches to treatment and care.
Early recognition and intervention can significantly improve the quality of life for individuals with diabetes, helping them manage their condition and prevent complications.
If you or someone you know is experiencing symptoms of diabetes, it is essential to seek medical advice for proper diagnosis and management.
FAQS (Frequently Asked Questions)
1: What is the difference between Type 1 and Type 2 diabetes?
Type 1 diabetes is an autoimmune condition where the immune system mistakenly attacks insulin-producing cells in the pancreas. This results in little to no insulin production, requiring lifelong insulin therapy. It often develops in children and young adults.
On the other hand, type 2 diabetes typically develops in adults and is characterized by insulin resistance, where the body’s cells do not respond effectively to insulin. Initially, the pancreas compensates by producing more insulin, but over time, it may not keep up with demand, leading to high blood sugar levels.
2: What are the symptoms of Type 1 and Type 2 diabetes?
Type 1 diabetes symptoms often develop rapidly and include increased thirst, frequent urination, extreme hunger, unintended weight loss, fatigue, and blurred vision. In contrast, Type 2 diabetes symptoms may develop gradually and include similar symptoms such as increased thirst and urination, fatigue, blurred vision, and slow wound healing.
However, some people with Type 2 diabetes may not experience noticeable symptoms initially, making regular screenings important, especially for those at risk.
3: How is Type 1 Diabetes managed compared to Type 2 Diabetes?
Managing Type 1 diabetes requires lifelong insulin therapy through injections or an insulin pump. Patients also need to monitor blood sugar levels regularly, adjust insulin doses based on food intake and physical activity, and maintain a balanced diet. Type 2 diabetes management focuses on lifestyle changes such as adopting a healthy diet, regular exercise, and maintaining a healthy weight.
Medications to improve insulin sensitivity or stimulate insulin production may also be prescribed. Some people with Type 2 diabetes may eventually require insulin therapy if other treatments are not sufficient.
4: What are the risk factors for Type 1 and Type 2 Diabetes?
Type 1 diabetes risk factors include family history, genetics, and autoimmune conditions. It is not preventable and typically manifests in childhood or adolescence.
Type 2 diabetes risk factors include being overweight or obese, lack of physical activity, unhealthy diet, older age, family history of diabetes, and certain ethnicities (e.g., African American, Hispanic/Latino, Native American).
Lifestyle changes can help reduce the risk of Type 2 diabetes, particularly maintaining a healthy weight, regular physical activity, and a balanced diet.
5: Can Type 1 diabetes develop into Type 2 diabetes, or vice versa?
Type 1 diabetes does not develop into Type 2 diabetes, as they are distinct conditions with different underlying causes. However, people with Type 1 diabetes may develop insulin resistance over time due to factors like weight gain or aging, requiring adjustments in management.
Conversely, Type 2 diabetes does not typically progress into Type 1 diabetes. Individuals can have both types of diabetes simultaneously, a condition known as double diabetes, where insulin resistance coexists with the autoimmune destruction of insulin-producing cells.
Proper diagnosis and individualized management are crucial for both types of diabetes to maintain optimal health and quality of life.




