Prediabetes is a condition characterized by higher than normal blood sugar levels, but not high enough to be diagnosed as type 2 diabetes. It’s often a warning sign that, if left unaddressed, can progress to full-blown diabetes.
However, the good news is that prediabetes can often be reversed or significantly delayed through lifestyle changes and careful management.
In this article, we’ll explore prediabetes in detail, its risk factors, and effective strategies for prevention.
What is Prediabetes?
Prediabetes is a critical stage that precedes the onset of type 2 diabetes. Fortunately, it offers an opportunity for individuals to make lifestyle changes and prevent the progression to full-blown diabetes. In this article, we will explore key strategies to manage prediabetes effectively and reduce the risk of developing Type 2 diabetes.
Prediabetes occurs when blood sugar levels are higher than normal but not yet high enough to be diagnosed as Type 2 diabetes. It serves as a warning sign, signaling the need for proactive measures to prevent further complications.
Blood sugar levels that are higher than normal but not high enough for a doctor to diagnose diabetes are known as prediabetes or borderline diabetes.
Prediabetes is almost always present before type 2 diabetes. However, symptoms are typically absent from it. Over 80% of the 98 million Americans who have prediabetes are unaware that they have the condition.
Treatment for prediabetes can avert more severe health issues, such as type 2 diabetes, and problems with your heart, blood vessels, kidneys, eyes, and eyes.
Your physician may also refer to this as:
- Impaired glucose tolerance (IGT)
- Impaired fasting glucose (IFG)
- Impaired glucose regulation (IGR)
- Non-diabetic hyperglycemia
Prediabetes Symptoms
Typically, there are no symptoms or indicators linked to prediabetes.
Darker skin on specific body areas could be an indication of prediabetes. The throat, underarms, and groin are possible affected locations.
The following classic indicators and symptoms indicate a transition from prediabetes to type 2 diabetes:
- Increased thirst
- Frequent urination
- Increased hunger
- Fatigue
- Blurred vision
- Numbness or tingling in the feet or hands
- Frequent infections
- Slow-healing sores
- Unintended weight loss
Symptoms of prediabetes in women
Among the early signs of diabetes mellitus that may specifically affect women (and those assigned female at birth) are:
- Yeast and urinary tract infections
- Longer and heavier periods
- Reduced interest in sex
- Vaginal dryness can make sex uncomfortable
- Trouble getting pregnant
Several of these symptoms can be mild and easily missed, so it’s vital to remember that. Testing blood sugar levels regularly is essential for identifying prediabetes, particularly in people with risk factors.
Causes of Prediabetes
Unknown is the specific cause of prediabetes. However, it seems that genetics and family history are significant factors. Individuals with prediabetes are no longer able to digest sugar or glucose effectively.
Food is the primary source of glucose in your body. Sugar is released into your circulation during digestion. Insulin decreases blood sugar levels by allowing sugar to enter your cells.
The pancreas is a gland that sits beneath the stomach and produces insulin. When you eat, your pancreas releases insulin into your bloodstream. The pancreas lowers blood sugar levels by decreasing the amount of insulin secreted into the bloodstream.

This method is not as effective in people with prediabetes. This means that instead of providing energy to your cells, sugar accumulates in your blood.
Insulin resistance causes you to develop prediabetes. That’s what happens when your body produces insulin incorrectly, a hormone that helps control blood sugar levels. Your blood sugar levels rise as a result, which is not healthy.
What causes insulin resistance?
The exact causes of insulin resistance in humans are unknown to medical professionals. However, factors that may be involved in it include:
- Your genetic makeup
- Overweight
- Prolonged stress
- loss of sleep
- Absence of exercise
- Consuming a lot of processed meals
- Certain hormonal diseases include hypothyroidism and Cushing’s syndrome
- Certain treatments include long-term use of steroid substances
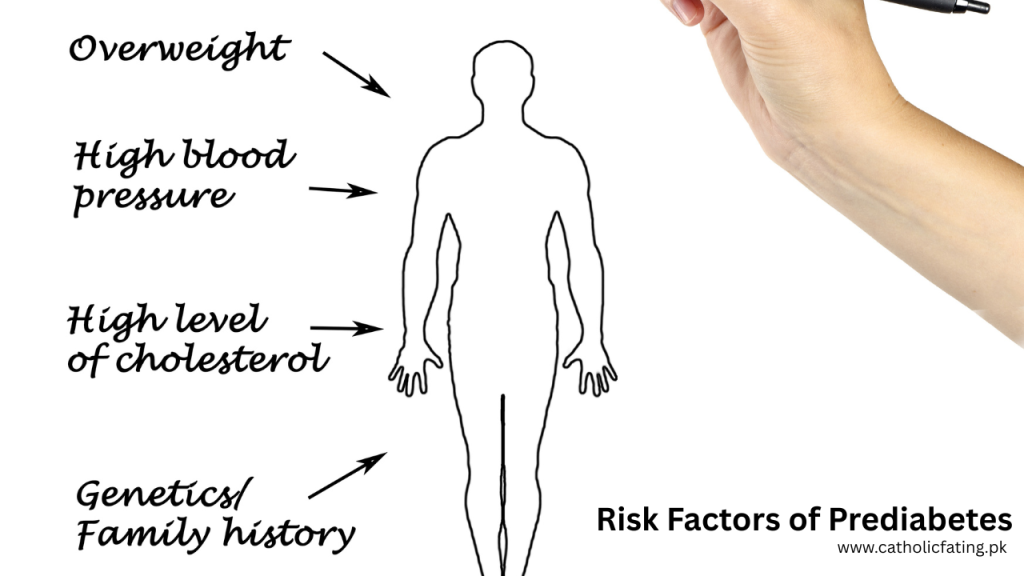
Risk Factors of Prediabetes
Blood sugar levels that are increased but not high enough to be considered type 2 diabetes are the hallmark of prediabetes. Although prediabetes may not cause as many acute health problems as diabetes, if left untreated, it greatly raises the risk of type 2 diabetes, heart disease, and stroke.
For prediabetes to be effectively managed, it is essential to identify the risk factors linked to the illness and take preventive measures.
- Sedentary Lifestyle: One of the primary risk factors for prediabetes is leading a sedentary lifestyle. Lack of physical activity contributes to weight gain and insulin resistance, both of which are key factors in the development of prediabetes. Regular physical activity helps improve insulin sensitivity and glucose metabolism, reducing the risk of prediabetes.
- Obesity and Central Adiposity: Obesity, especially central adiposity (excess fat around the abdomen), significantly increases the risk of prediabetes. Fat accumulation around the abdomen, known as visceral fat, releases inflammatory substances that interfere with insulin action, leading to insulin resistance. Body mass index (BMI) and waist circumference are important indicators of obesity-related prediabetes risk.
- Unhealthy Diet: Poor dietary habits, characterized by excessive consumption of sugary beverages, refined carbohydrates, saturated fats, and processed foods, are strongly associated with prediabetes. These foods contribute to weight gain, insulin resistance, and inflammation, exacerbating the risk of developing the condition. Conversely, a diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can help prevent prediabetes by promoting weight management and improving insulin sensitivity.
- Family History and Genetics: Genetic predisposition plays a significant role in the development of prediabetes. Individuals with a family history of type 2 diabetes are at higher risk of developing prediabetes themselves. Certain genetic variants can affect insulin production, glucose metabolism, and susceptibility to obesity, contributing to the onset of prediabetes. Understanding family history can help identify individuals at increased risk and guide preventive measures.
- Age and Ethnicity: Age is another risk factor for prediabetes, with the prevalence increasing with advancing age. As people age, muscle mass tends to decrease, and fat accumulation, especially around the abdomen, tends to increase, predisposing them to insulin resistance and prediabetes. Additionally, certain ethnicities, such as African American, Hispanic/Latino, Native American, Asian American, and Pacific Islander, have a higher predisposition to prediabetes and type 2 diabetes compared to Caucasians.
- Gestational Diabetes: Women who have experienced gestational diabetes (diabetes during pregnancy) are at increased risk of developing prediabetes and type 2 diabetes later in life. Gestational diabetes indicates impaired glucose tolerance during pregnancy, highlighting underlying insulin resistance and predisposing factors for future metabolic complications. Women with a history of gestational diabetes should undergo regular screening for prediabetes and adopt preventive measures to reduce their risk.
- Polycystic Ovary Syndrome (PCOS): PCOS is a common endocrine disorder characterized by hormonal imbalances, irregular menstrual cycles, and ovarian cysts. Women with PCOS have a higher prevalence of insulin resistance and are at increased risk of developing prediabetes and type 2 diabetes. Managing PCOS through lifestyle modifications, medication, and regular monitoring is essential to preventing the progression of prediabetes and diabetes.
To prevent prediabetes from progressing to type 2 diabetes and its associated implications, early management and identification of the risk factors associated with the condition are essential.
Reducing the risk of prediabetes mostly involves making lifestyle changes such as regular physical activity, good diet, managing weight, avoiding tobacco and excessive alcohol use, and managing weight.
An increased risk of prediabetes is also linked to the following conditions:
- Increased Blood Pressure
- Low amounts of HDL cholesterol, or “good” cholesterol, are present.
- High Blood Triglyceride levels, a kind of fat
Also, preventing the formation of prediabetes and enhancing long-term health outcomes requires targeted screening and tailored therapies for high-risk individuals, such as those with a history of gestational diabetes or diabetes in the family.
Through the management of modifiable risk factors and the implementation of preventive interventions, people can proactively take charge of their health and lower their chances of developing prediabetes and its consequences.
Key Strategies to Manage Prediabetes:
Blood sugar levels that are higher than normal but not high enough to be categorized as type 2 diabetes are known as prediabetes. Proactive actions can stop or postpone the onset of diabetes during this important phase. To effectively manage prediabetes, blood sugar levels must be controlled, lifestyle modifications must be made, and the risk of type 2 diabetes and its related consequences must be decreased.

Here are some important strategies for controlling prediabetes:
1: Healthy Eating Habits:
- Emphasize a balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats.
- Monitor portion sizes to avoid overeating and maintain a healthy weight.
- Limit your intake of processed foods, sugary beverages, and high-fat foods.
- Incorporate fiber-rich foods to help regulate blood sugar levels and improve digestion.
2: Regular Physical Activity:
- Aim for at least 150 minutes of moderate-intensity aerobic exercise per week, such as brisk walking, swimming, or cycling.
- Include strength training exercises at least twice a week to build muscle mass and improve insulin sensitivity.
- Find activities you enjoy to stay motivated and make exercise a regular part of your routine.
- Stay active throughout the day by taking short walks, using stairs instead of elevators, and incorporating movement into daily tasks.
3: Weight Management:
- Achieve and maintain a healthy weight by following a balanced diet and engaging in regular physical activity.
- Set realistic weight loss goals and track progress over time.
- Aim for gradual weight loss of 1-2 pounds per week to ensure sustainable results.
- Consult with a healthcare provider or a registered dietitian to develop a personalized weight loss plan based on individual needs and preferences.
4: Monitor Blood Sugar Levels:
- Check blood sugar levels regularly using a glucometer or other monitoring devices as recommended by your healthcare provider.
- Keep track of your blood sugar readings and identify patterns to make necessary adjustments to your diet and lifestyle.
- Work with your healthcare team to establish target blood sugar levels and develop a monitoring schedule that fits your needs.
5: Stress Management:
- Practice stress-reducing techniques such as deep breathing, meditation, yoga, or tai chi to lower cortisol levels and improve insulin sensitivity.
- Prioritize self-care activities and make time for relaxation and leisure activities.
- Identify sources of stress in your life and develop coping strategies to manage them effectively.
6: Get Adequate Sleep:
- Aim for 7-9 hours of quality sleep per night to support overall health and well-being.
- Establish a regular sleep schedule and create a relaxing bedtime routine to promote better sleep hygiene.
- Avoid caffeine, alcohol, and electronic devices before bedtime, as they can interfere with sleep quality.
7: Regular Medical Check-ups:
- Schedule regular check-ups with your healthcare provider to monitor your prediabetes and overall health.
- Discuss any concerns or changes in symptoms with your healthcare team and follow their recommendations for treatment and management.
- Stay up-to-date with preventive screenings and vaccinations to reduce the risk of complications associated with prediabetes.
8: Medication Management (if prescribed):
- Follow your healthcare provider’s recommendations regarding medication management for prediabetes.
- Take prescribed medications as directed and communicate any side effects or concerns with your healthcare team.
- Monitor blood sugar levels regularly and report any significant changes to your healthcare provider.
Adopting healthy lifestyle practices, keeping an eye on blood sugar levels, and collaborating closely with medical providers are all essential components of a complete strategy for managing prediabetes.
People with prediabetes can take steps to lower their risk of type 2 diabetes and enhance their general health and well-being. It’s never too late to start taking charge of your health and making decisions that will benefit you now and in the future.
Gestational diabetes during pregnancy:
Gestational diabetes is a type of diabetes that develops during pregnancy. Most of the time, gestational diabetes goes away after your baby is born. Even if your gestational diabetes goes away, you still have a greater chance of developing type 2 diabetes within 5 to 10 years.
Your child may also be more likely to become obese and develop type 2 diabetes later in life. Making healthy choices helps the whole family and may protect your child from becoming obese or developing diabetes.
Steps you should take for yourself and your child if you have gestational diabetes:
- Get tested for diabetes 6 to 12 weeks after your baby is born. If your blood glucose is still high, you may have type 2 diabetes. If your blood glucose is normal, you should get tested every 3 years to see if you have developed type 2 diabetes.
- Be more active and make healthy food choices to get back to a healthy weight.
- Breastfeed your baby. Breastfeeding gives your baby the right balance of nutrients and helps you burn calories.
- Ask your doctor if you should take the diabetes drug metformin to help prevent type 2 diabetes.
Metabolic Disorder
Certain obesity-related diseases are linked to insulin resistance and can raise your chance of developing diabetes, heart disease, and stroke. Metabolic syndrome refers to a group of three or more of these conditions together:
- High blood pressure
- Low levels of HDL
- High triglycerides
- High blood sugar levels
- Large waist size
Complications of Prediabetes
Even if your type 2 diabetes has not yet developed, prediabetes has been associated with long-term harm, such as to your kidneys, blood vessels, and heart. Additionally, undetected (silent) heart attacks are associated with prediabetes.
Type 2 diabetes can develop from prediabetes, and this can result in:
- High blood pressure
- High cholesterol
- Heart disease
- Stroke
- Kidney disease
- Nerve damage
- Fatty liver disease
- Eye damage, including loss of vision
- Amputations
Prevention of Prediabetes
Blood sugar levels that are higher than normal but not high enough to be classified as type 2 diabetes are known as prediabetes. Uncontrolled prediabetes raises the chance of type 2 diabetes, which enhances the risk of numerous health issues. Still, prediabetes can frequently be treated with a lifestyle change.

Even if diabetes runs in your family, you can prevent prediabetes and the condition’s progression to type 2 diabetes by leading a healthy lifestyle. Among them are:
1: Eating Healthy Foods:
- Emphasize Whole Foods: Base your diet on whole, unprocessed foods such as fruits, vegetables, whole grains, lean proteins, and healthy fats. These foods are rich in nutrients and fiber, which help regulate blood sugar levels and improve insulin sensitivity.
- Limit Sugary and Processed Foods: Minimize consumption of sugary beverages, refined carbohydrates, and processed foods high in added sugars and unhealthy fats. These foods can cause spikes in blood sugar and contribute to insulin resistance.
- Portion Control: Pay attention to portion sizes to prevent overeating, which can lead to weight gain and worsen insulin resistance. Use smaller plates, measure serving sizes, and avoid eating straight from large packages.
2: Getting Active:
- Regular Exercise: Aim for at least 150 minutes of moderate-intensity aerobic exercise or 75 minutes of vigorous-intensity exercise per week, as recommended by health guidelines. Incorporate activities you enjoy, such as walking, cycling, swimming, or dancing.
- Strength Training: Include strength training exercises at least twice a week to build muscle mass, which can help improve insulin sensitivity and glucose metabolism.
- Stay Active Throughout the Day: Break up long periods of sitting with short bouts of activity. Take walking breaks, use stairs instead of elevators, and find opportunities to move whenever possible.
3: Losing Excess Weight:
- Set Realistic Goals: Aim for gradual weight loss of 1-2 pounds per week through a combination of dietary changes and increased physical activity. Set achievable goals to avoid becoming discouraged.
- Balanced Diet: Focus on creating a calorie deficit by consuming fewer calories than you expend. Choose nutrient-dense foods that provide satiety while supporting weight loss efforts.
- Seek Support: Consider working with a registered dietitian or a certified personal trainer to develop a personalized plan tailored to your needs and goals. Joining a support group or involving friends and family can also provide encouragement and accountability.
4: Controlling Blood Pressure and Cholesterol:
- Monitor Blood Pressure: Regularly check your blood pressure and take steps to keep it within a healthy range. This may include following a low-sodium diet, engaging in regular physical activity, managing stress, and, if necessary, taking prescribed medications.
- Maintain Healthy Cholesterol Levels: Keep cholesterol levels in check by adopting a heart-healthy diet low in saturated and trans fats. Include foods rich in omega-3 fatty acids, such as fatty fish, nuts, and seeds. Regular exercise and avoiding smoking also support healthy cholesterol levels.
- Regular Health Checkups: Schedule regular checkups with your healthcare provider to monitor your blood pressure, cholesterol, and overall health. Discuss any concerns or questions you have about managing these risk factors for prediabetes and diabetes.
5: Not Smoking:
- Quit Smoking: If you smoke, quitting is one of the best things you can do for your overall health. Smoking increases the risk of insulin resistance, type 2 diabetes, heart disease, and other serious health conditions.
- Seek Support: Quitting smoking can be challenging, but there are resources available to help you quit successfully. Consider enrolling in a smoking cessation program, using nicotine replacement therapy, or seeking support from friends, family, or healthcare professionals.
- Focus on Healthy Coping Strategies: Find alternative ways to cope with stress and manage cravings, such as exercising, practicing relaxation techniques, or engaging in hobbies and activities you enjoy. Surround yourself with supportive individuals who encourage your efforts to quit smoking.
Developing healthy lifestyle behaviors and controlling risk factors, including smoking, high blood pressure, high cholesterol, and excess weight, are only a few of the many components of an extensive approach needed to prevent prediabetes.
You may lower your risk of having prediabetes and the difficulties that come with it by gradually changing your diet, increasing your physical activity, keeping a healthy weight, keeping an eye on important health indicators, and giving up smoking.
Keep in mind that making modest, regular changes to your lifestyle can have a big long-term impact on your general health and well-being.
Prediabetes Tests and Diagnosis
The following tests are among the ones your doctor will perform:
Fasting Plasma Glucose Test
After eight hours of fasting, a technician will draw blood to measure your blood sugar levels.
Results show:
- Normal range if your blood sugar is less than 100 milligrams per deciliter (mg/dL)
- Prediabetes range if your blood sugar is 100-125 mg/dL
- Diabetes range if your blood sugar is 126 mg/dL or higher
Oral Glucose Tolerance Test
Your plasma glucose will be tested after a fast. After that, you’ll sip on something sweet. More blood will be collected for testing by a professional after two hours. The findings show:
- Normal range if your blood sugar is less than 140 mg/dL after the second test
- Prediabetes range if your blood sugar is 140-199 mg/dL after the second test
- Diabetes range if your blood sugar is 200 mg/dL or higher after the second test
What should I do if I feel I’m suffering from prediabetes?
Prediabetes is when your blood glucose, also called blood sugar, levels are higher than normal, but not high enough to be called diabetes. Having prediabetes is serious because it raises your chances of developing type 2 diabetes. Many of the same factors that raise your chance of developing type 2 diabetes put you at risk for prediabetes.
Other names for prediabetes include impaired fasting glucose or impaired glucose tolerance. Some people call prediabetes “borderline diabetes.”
About 1 in 3 Americans has prediabetes, according to recent diabetes statistics External link from the Centers for Disease Control and Prevention. You won’t know if you have prediabetes unless you are tested.
If you have prediabetes, you can lower your chance of developing type 2 diabetes. Lose weight if you need to, become more physically active, and follow a reduced-calorie eating plan.
Get started with Your Game Plan to Prevent Type 2 Diabetes. For more support, you can find a lifestyle change program near you through the National Diabetes Prevention Program.
Conclusion:
Managing prediabetes involves a holistic approach that includes adopting a healthy lifestyle, maintaining a balanced diet, engaging in regular physical activity, and addressing factors like stress and sleep.
By implementing these key strategies, individuals with prediabetes can significantly reduce their risk of progressing to Type 2 Diabetes and enjoy long-term health benefits.
It’s important to work closely with healthcare professionals to develop a personalized plan tailored to individual needs and circumstances.
At Catholic Fating, Prediabetes is a wake-up call. Make healthy changes now to prevent type 2 diabetes.
FAQS (Frequently Asked Questions)
1: What is prediabetes?
Prediabetes is a health condition characterized by higher-than-normal blood sugar levels, but not high enough to be classified as type 2 diabetes. It’s considered a warning sign that indicates a person is at risk of developing type 2 diabetes if preventive measures are not taken. In prediabetes, blood sugar levels are higher than normal, but not yet high enough to be diagnosed as diabetes.
2: What are the symptoms of prediabetes?
Prediabetes typically doesn’t present with noticeable symptoms. Most people with prediabetes are asymptomatic, which is why it’s often referred to as a “silent” condition. However, some individuals may experience symptoms such as increased thirst, frequent urination, fatigue, and blurred vision. Since these symptoms can be mild and easily attributed to other factors, prediabetes is often detected through routine blood tests during check-ups.
3: What are the risk factors for prediabetes?
Several factors can increase your risk of developing prediabetes. These include being overweight or obese, having a family history of diabetes, leading a sedentary lifestyle with little to no physical activity, and having high blood pressure or high cholesterol levels. Additionally, certain ethnicities, such as African American, Hispanic/Latino, Native American, Asian American, and Pacific Islander, are at higher risk of developing prediabetes.
4: How is prediabetes diagnosed?
Prediabetes is diagnosed through blood tests that measure blood glucose levels. The most common test used to diagnose prediabetes is the fasting plasma glucose (FPG) test, which measures blood sugar levels after an overnight fast. Another test is the oral glucose tolerance test (OGTT), where blood sugar levels are measured before and after consuming a sugary drink. Additionally, the A1C test provides an average of blood sugar levels over the past two to three months.
5: Can prediabetes be reversed?
Yes, prediabetes can often be reversed or delayed through lifestyle changes such as adopting a healthy diet, increasing physical activity, and losing weight if overweight or obese. A balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can help control blood sugar levels. Regular exercise, aiming for at least 150 minutes of moderate-intensity aerobic activity per week, can also improve insulin sensitivity and blood sugar control.
Additionally, quitting smoking and limiting alcohol intake can further reduce the risk of developing type 2 diabetes. In some cases, medication may be prescribed by a healthcare provider to help manage blood sugar levels in conjunction with lifestyle changes. Regular monitoring of blood sugar levels and follow-up with healthcare providers are crucial for managing prediabetes effectively.




