Gestational diabetes, a form of diabetes that develops during pregnancy, can have significant implications for both the mother and the baby.
One of the key aspects of managing gestational diabetes is closely monitoring blood sugar levels to ensure they remain within target ranges.
In this article, we’ll explore the importance of blood sugar monitoring in gestational diabetes and provide detailed guidance on how to monitor blood sugar levels during pregnancy effectively.
WHAT IS GESTATIONAL DIABETES?
Gestational diabetes is a type of diabetes that can develop during pregnancy in individuals who don’t already have diabetes. The Centers for Disease Control and Prevention (CDC) estimates that gestational diabetes affects between 2 and 10 percent of pregnancies in the United States. It usually goes away after delivery.
Normally, the body uses a hormone called insulin to turn blood sugar (glucose) into energy. During pregnancy, the placenta produces hormones that can make it harder for the body’s cells to use insulin, causing blood sugar levels to rise.

Gestational diabetes usually develops in the second trimester of pregnancy, between 24 and 28 weeks. If left untreated, it can increase the risk of health problems for both the mother and the baby. However, with proper management, most women with gestational diabetes can have a healthy pregnancy and baby.
Here are some risk factors for gestational diabetes:
- Being overweight or obese before pregnancy
- Having a family history of diabetes
- Having had gestational diabetes in a previous pregnancy
- Being older than 25 years old
- Having a personal history of polycystic ovary syndrome (PCOS)
High blood sugar levels can affect your baby’s health. If you have gestational diabetes, you’ll need to monitor your blood sugar levels and work with your doctor to keep them under control. You can have a healthy pregnancy and a healthy baby with good management.
Why DOES GESTATIONAL DIABETES OCCUR?
Insulin is a hormone that enables glucose (sugar) in the bloodstream to enter the body’s cells. Sugar is the source of energy for cells. During pregnancy, the fetus and placenta produce hormones that make the pregnant individual resistant to insulin.
Most pregnant individuals can produce enough extra insulin to compensate for this, thus keeping their blood sugar level normal. However, some cannot, so their blood sugar level rises, resulting in gestational diabetes.
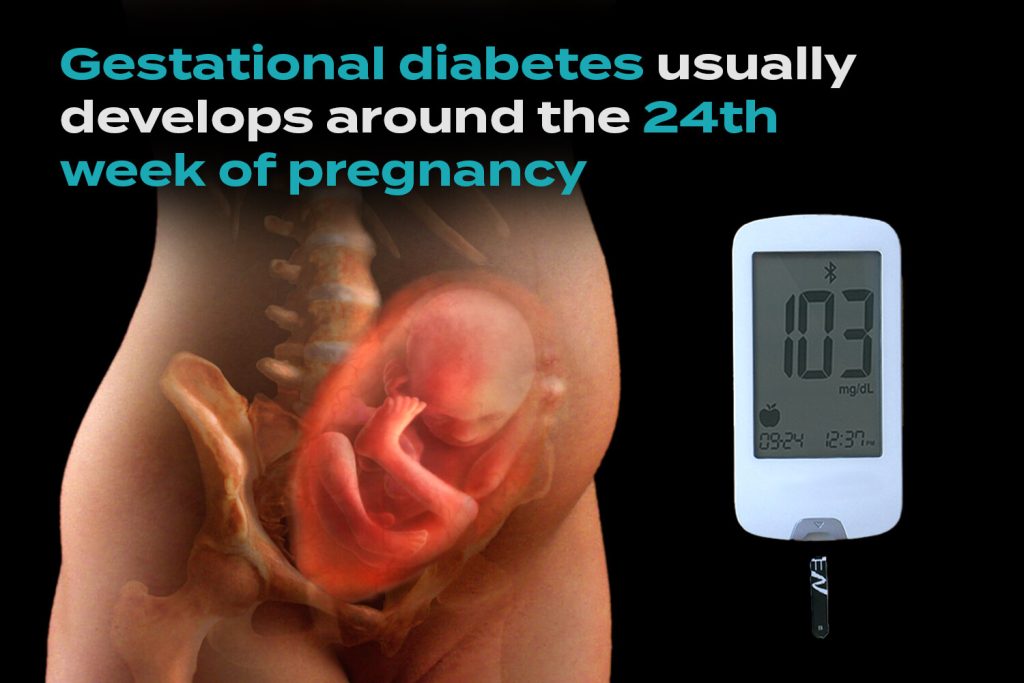
Gestational diabetes develops due to a combination of hormonal changes and your body’s response to those changes during pregnancy. Here’s a breakdown:
- Insulin and Blood Sugar: Insulin, a hormone produced by your pancreas, acts like a key, unlocking your cells to absorb blood sugar (glucose) for energy. Normally, your body adjusts insulin production to maintain healthy blood sugar levels.
- Pregnancy Hormones: During pregnancy, the placenta produces hormones that help your baby grow. However, some of these hormones can interfere with insulin’s ability to work effectively. This is called insulin resistance.
- Increased Insulin Demand: Due to insulin resistance, your body needs to produce more insulin to keep blood sugar under control.
- Insufficient Insulin Production: In some cases, the body can’t produce enough extra insulin to overcome the pregnancy hormones’ effects. This situation leads to gestational diabetes.
WHY IS GESTATIONAL DIABETES IMPORTANT?
The diagnosis and treatment of gestational diabetes are important to minimize the risk of complications from the disorder.
Complications of gestational diabetes can include:
- Giving birth to a large baby (weighing more than 9.0 lbs or 4.1 kg), eases the risk of injury to the pregnant individual or baby during birth and increases the chance of needing a cesarean birth. Large babies born to individuals with gestational diabetes can be at increased risk of developing diabetes and obesity during their lifetime.
- Newborn hypoglycemia (low blood sugar in the newborn period).
- Preeclampsia (a type of high blood pressure during pregnancy). (See “Patient education: Preeclampsia (Beyond the Basics)”.)
- Stillbirth (a baby who dies before being born), is a complication that, fortunately, is now rare in individuals with gestational diabetes because of good control of blood sugars and careful monitoring of them and their babies during pregnancy.
Furthermore, those with gestational diabetes are at high risk of developing pre-diabetes (impaired glucose tolerance) or type 2 diabetes when they are no longer pregnant, so they need to be tested for diabetes postpartum and in the years after giving birth.
Blood Sugar Monitoring in Gestational Diabetes Testing
We recommend that all pregnant individuals get tested for gestational diabetes.
Timing of test: Testing for gestational diabetes is usually done once between 24 and 28 weeks of pregnancy. However, testing for diabetes may be done as early as your first prenatal visit if you have risk factors for diabetes, such as:
- A history of gestational diabetes in a previous pregnancy
- Obesity
- A strong family history of diabetes
- Polycystic ovarian syndrome (PCOS)
Test procedure: There are a few ways to test for gestational diabetes.
- Two-part test: On the day of the screening test, you can eat and drink normally. You will be given 50 grams of glucose, usually in the form of a specially formulated orange or cola drink. You should drink the entire amount within a few minutes. One hour later, you will have a blood test to measure your blood sugar levels in gestational diabetes.
If your blood sugar level is normal, no other tests are done.
Most doctors and nurses consider your blood sugar level in the screening test to be high if it is above 130 to 140 mg/dL (7.2 to 7.7 mmol/L). If your blood sugar level is very high (≥200 mg/dL [11.1 mmol/L]), there is a very strong chance that you have gestational diabetes.
Oral Glucose Tolerance Test
If your screening test blood sugar level is high but not very high, you will need another test to know for sure if you have gestational diabetes. This test is called an oral glucose tolerance test (GTT).
- The test is done by measuring your blood sugar level before you eat or drink anything in the morning (fasting), then again one, two, and three hours after you drink a glucose drink that contains 100 grams of glucose (twice the amount in the one-hour test). Similar to the one-hour test, this is usually in the form of a specially formulated orange, lemon-lime, or cola drink.
Gestational diabetes is diagnosed if you have two or more elevated blood sugar values during the GTT, although some doctors may recommend treatment after a single elevated value, especially if you have other signs of gestational diabetes (a big fetus or extra fluid around your fetus).
- One-part test: Some doctors and nurses test for diabetes with a one-part test. The test is done by measuring your blood sugar level before you eat or drink anything in the morning (fasting), then again one and two hours after you drink a glucose drink that contains 75 grams of glucose. This is usually in the form of a specially formulated orange, lemon-lime, or cola drink.
Gestational diabetes is diagnosed if you have one or more elevated blood sugar values.
GESTATIONAL DIABETES TREATMENT
After you are diagnosed with gestational diabetes, you will need to make changes in what you eat and learn to check your blood sugar level. You may also be advised to get more exercise. If changing your diet and activity doesn’t result in normal blood sugar levels, you will also need to learn how to give yourself insulin injections or take a pill to lower your blood sugar levels.
The main goal of treatment for gestational diabetes is to reduce the risk of complications such as those mentioned above. One of the main complications is an overly large baby (weighing more than 9 to 10 lbs at birth). You are more likely to have a large baby if your blood sugar levels are higher than normal during pregnancy.
A large baby can be difficult to deliver vaginally. The baby can get stuck after the head is born (called “shoulder dystocia”). This increases the risk of injury to the baby (eg, broken bones or nerve injury) and to the mother (eg, more severe vaginal tears). If labor does not progress normally, you may need a cesarean birth.
Eating plan: The first treatment for gestational diabetes is eating right. To help you achieve the changes you should make in your diet, you will meet with a dietitian, nurse, or certified diabetic educator (a nurse or dietician that specializes in diabetes).
The general guidelines below will help you until you receive your individualized food plan.
- Continue to eat a healthy pregnancy diet.
- Avoid sweet desserts and presweetened beverages. This includes candy, cake, cookies, ice cream, donuts, jams and jellies, syrups, and sweet sauces. Also, avoid adding sugar to your food or drinks, such as sweetened soda, punch, sweet tea, and other fruity beverages.
- You may use the alternative sweeteners aspartame (Nutrasweet), sucralose (Splenda), stevioside (Stevia), or acesulfame potassium (Sunnet). Moderation is suggested. These sweeteners have not been linked to an increased risk of congenital anomalies (birth defects).
- Include protein with limited saturated fat, such as trimmed red meat and pork, chicken, and fish (limit types and amounts of fish due to mercury concerns). Other protein foods, like cheese, eggs, nuts, seeds, and peanut butter, are also good for you and your baby.
- Eat moderate portions of carbohydrates (natural starches and sugars) containing foods.
- Starchy foods (eg, breads, rice, pasta, potato, corn, cereals): Choose whole grains over refined grains when possible.
- Fruits and fruit juices: Limit fruit servings to a small piece of fruit or approximately 1 cup at a time. Avoid fruit juice, or limit 100 percent fruit juice to one-half cup (4 ounces) per serving. Many dieticians recommend avoiding fruits for breakfast because of concerns about higher blood sugar levels in the early morning.
- Milk and yogurt – Skim or 1 percent milk is healthiest. Choose low-fat yogurt that is plain, “light,” or Greek style.
- Many vegetables are low in sugar and carbohydrates. Include plenty of salads, greens (spinach, collards, kale), broccoli, carrots, green beans, tomatoes, onions, mushrooms, and other vegetables you enjoy. Half of the plate at your meals can be non-starchy vegetables.
- Use healthy fats, like olive or canola oil.
Blood Sugar Monitoring in Gestational Diabetes — You will learn how to check your blood sugar level and record the results (Figure 1). Instructions for choosing a blood sugar meter, checking blood sugar levels at home, and ways to record the results are discussed separately. (See “Patient education: Glucose monitoring in diabetes (Beyond the Basics)”.)
Initially, most individuals should check their blood sugar level four times per day:
- Before eating in the morning
- One or two hours after the first bite of food with breakfast, lunch, and dinner.
This information can help to determine whether your blood sugar levels are on target. If your levels stay higher than they should be, your doctor will probably recommend that you start using insulin. (See ‘Insulin’ below.)
Exercise — Although exercise is not a necessary part of gestational diabetes treatment, it might help to control blood sugar levels. If you were exercising before, you should continue after being diagnosed with gestational diabetes.
If you did not previously exercise, ask your doctor or nurse if exercise is recommended. Most individuals who do not have medical or pregnancy-related complications can exercise, at least moderately, throughout their pregnancy. Walking is a great form of exercise for those starting an exercise regimen.
Insulin: Approximately 15 percent of patients with gestational diabetes will require insulin. Insulin is a medicine that helps to reduce blood sugar levels and can reduce the risk of gestational diabetes-related complications. Insulin is the most common medicine for treating gestational diabetes.
You must give insulin by injection because it does not work when it is taken by mouth. Most pregnant people start by giving one to two shots of insulin per day. If your blood sugar levels are high after eating, you may need to give yourself a shot three or four times per day. Instructions for drawing up and giving insulin shots are available separately.
If you take insulin, you should check your blood sugar level at least four times per day. You also need to write down your results (or store them in the meter) and how much insulin you took, and review these records at each prenatal visit or more frequently based on your doctor’s recommendation.
Keeping accurate records helps to adjust insulin doses and can decrease the risk of complications.
If you take insulin, you should also:
- Eat three small-sized meals and three to four healthy snacks.
- Eat every two to three hours to space food evenly throughout your day.
- Do not skip meals or snacks. The bedtime snack is especially important to help keep your fasting (first blood sugar of the day before eating) in check.
Oral Diabetes Medicines
such as those taken by people with type 2 diabetes, are sometimes used during pregnancy in the United States. We prefer insulin therapy for pregnant patients with diabetes who cannot control blood glucose levels adequately by their diet (nutritional therapy). Insulin is effective and safe and does not cross the placenta to the fetus.
Most oral diabetes medicines pass from the pregnant individual to their baby through the placenta; while they have not been shown to harm the fetus or newborn, it is not known if there are longer-term effects on children. T
Here are studies underway to help answer this question. However, oral anti-hyperglycemic agents are a reasonable alternative for individuals who will not take, or are unable to comply with, insulin therapy, as long as they understand the lack of information on long-term risks or benefits
MONITORING DURING PREGNANCY
- Prenatal visits — Most pregnant individuals who develop gestational diabetes have more frequent prenatal visits (eg, once every week or two), especially if insulin is used. The purpose of these visits is to monitor your and your baby’s health, discuss your diet, review your blood sugars, and adjust your dose of insulin (if you are taking it) to keep your blood sugar levels near normal. It is common to change the dose of insulin as the pregnancy progresses. You may also be asked to have one or two ultrasound examinations to check on the growth and size of the baby. (See “Gestational diabetes mellitus: Obstetric issues and management”.)
- Nonstress testing: You may need tests to monitor the health of the baby during the later stages of pregnancy, especially if your blood sugars have been high, you are using insulin, or if you have any pregnancy-related complications (eg, high blood pressure). The most commonly used test is the nonstress test. This test is discussed in a separate topic review.
LABOR AND DELIVERY WITH GESTATIONAL DIABETES
If your blood sugar levels are close to normal during pregnancy and you have no other complications, the ideal time to give birth is between 39 and 40 weeks of pregnancy, no later than your due date.
If you do not give birth by your due date, you may be offered induction of labor or additional testing to monitor your and your baby’s health. (See “Patient education: Postterm pregnancy (Beyond the Basics)”.)
In most individuals with gestational diabetes and a normal-size baby, there are no advantages to a cesarean over a vaginal birth, although cesarean may be needed in any pregnancy, especially with a first baby. Those with a very large baby may be offered cesarean birth before labor starts. The risks and benefits of cesarean birth are discussed separately. (See “Patient education: C-section (cesarean delivery) (Beyond the Basics)”.)
Your blood sugar levels will be monitored during labor. Most individuals have normal blood sugar levels during labor and do not need any insulin. Insulin is given if your blood sugar level becomes high. High blood sugar levels during labor can cause problems in the baby, both before and after delivery.
AFTER-DELIVERY CARE
After giving birth, most individuals with gestational diabetes have normal blood sugar levels and do not require further treatment with insulin. You can return to your prepregnancy diet, and you are encouraged to breastfeed.
However, your doctor may check your blood sugar level the day after delivery to be sure that it is normal or near normal. Pregnancy itself does not increase the risk of developing type 2 diabetes. However, having gestational diabetes mellitus does increase your risk of developing type 2 diabetes later in life.
After you deliver, you should have testing for type 2 diabetes. Typically, this is done between 4 and 12 weeks postpartum, ideally before your postpartum check-up. But it may be done in the hospital before you are discharged. Testing usually includes a two-hour glucose tolerance test (GTT) so that you are tested for both pre-diabetes and diabetes.
- Risk of recurrent gestational diabetes — One-third to two-thirds of individuals who have gestational diabetes in one pregnancy will have it again in a later pregnancy. If you are overweight or obese, weight reduction through diet and exercise can reduce this risk.
- Risk of developing type 2 diabetes — Individuals with gestational diabetes have an increased risk of developing type 2 diabetes later in life, especially if they have other risk factors (eg, family history of type 2 diabetes).
The risk of developing type 2 diabetes is greatly affected by body weight. Individuals with obesity have a 50 to 75 percent risk of developing type 2 diabetes, while this risk is less than 25 percent in those who are of a normal weight. If you are overweight or obese, you can reduce your risk of type 2 diabetes by losing weight and exercising regularly.
The American Diabetes Association (ADA) recommends that all persons with a history of gestational diabetes have testing for type 2 diabetes every one to three years after their initial post-pregnancy test for diabetes. If you have elevations in your blood sugars in the pre-diabetes range at the time of your postpartum screening, the ADA recommends yearly testing. It is also recommended that you work with your primary care provider to eat a healthy diet, lose any excess weight, and exercise regularly to help decrease your risk of developing type 2 diabetes.
- Cardiovascular disease — Individuals who have had gestational diabetes in the past are at increased risk of developing cardiovascular disease, including heart attack and stroke. While this is mostly tied to the risk of type 2 diabetes (see above), even those who do not develop type 2 diabetes appear to have a small increase in their risk of heart disease later in life. Continuing to make healthy lifestyle choices such as eating a balanced diet, exercising regularly, and avoiding smoking can help minimize this risk. (See “Type 2 Diabetes: Taking Control of Your Type 2 Diabetes Journey”.)
- Birth control — Individuals with a history of gestational diabetes can use any type of birth control after pregnancy. A review of all of the birth control options is available separately.
Interpreting Blood Sugar Readings
Interpreting blood sugar readings is crucial for effective management of gestational diabetes. Target blood sugar ranges may vary depending on individual circumstances, but in general, the following guidelines are often recommended:
- Fasting Blood Sugar: Typically, the target range for fasting blood sugar levels is between 60 and 95 mg/dL (3.3 to 5.3 mmol/L).
- Pre-Meal Blood Sugar: Target ranges for pre-meal blood sugar levels are often between 60 and 99 mg/dL (3.3 to 5.5 mmol/L).
- Postprandial Blood Sugar: Blood sugar levels one to two hours after meals should ideally be below 140 mg/dL (7.8 mmol/L).
It’s essential to work closely with healthcare providers to establish personalized target ranges based on individual health status and treatment goals.
Conclusion
Blood sugar monitoring is a cornerstone of gestational diabetes management, allowing for timely adjustments to treatment plans and optimization of glycemic control.
Through methods such as SMBG, CGM, and periodic HbA1c testing, pregnant women with gestational diabetes can maintain optimal blood sugar levels, reducing the risk of complications for both themselves and their babies.
By adhering to recommended monitoring protocols and working closely with healthcare providers, women with gestational diabetes can navigate their pregnancies safely and ensure the best possible outcomes for themselves and their babies.
FAQS (Frequently Asked Questions)
1: What is gestational diabetes, and why is monitoring blood sugar important during pregnancy?
Gestational diabetes is a type of diabetes that develops during pregnancy, typically around the 24th to 28th week. Monitoring blood sugar levels is crucial to ensure the mother and baby’s health, as uncontrolled blood sugar levels can lead to complications such as macrosomia (large birth weight), preterm birth, and increased risk of cesarean delivery.
2: How often should blood sugar levels be monitored for women with gestational diabetes?
Blood sugar levels should typically be monitored multiple times a day, as recommended by the healthcare provider. This often involves checking fasting blood sugar levels in the morning and after meals, aiming to keep levels within a target range to manage gestational diabetes effectively.
3: What are the target blood sugar levels for women with gestational diabetes?
Target blood sugar levels may vary depending on individual circumstances and healthcare provider recommendations. However, typical targets for fasting blood sugar levels are often between 60-95 mg/dL (3.3-5.3 mmol/L), and postprandial (after-meal) levels may be around 100-120 mg/dL (5.5-6.7 mmol/L).
4: How can diet and lifestyle changes help in managing blood sugar levels during gestational diabetes?
Adopting a balanced diet rich in whole grains, fruits, vegetables, lean proteins, and healthy fats can help regulate blood sugar levels. Additionally, regular physical activity, under the guidance of a healthcare provider, can improve insulin sensitivity and aid in managing blood sugar levels during gestational diabetes.
5: What should I do if my blood sugar levels are consistently out of the target range despite following dietary and lifestyle recommendations?
If blood sugar levels remain consistently high or low despite dietary and lifestyle modifications, it’s essential to consult with a healthcare provider. They may adjust the treatment plan, which could include medication such as insulin injections, to help maintain blood sugar levels within the target range for a healthy pregnancy.




